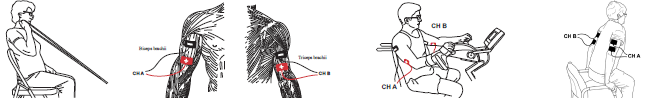
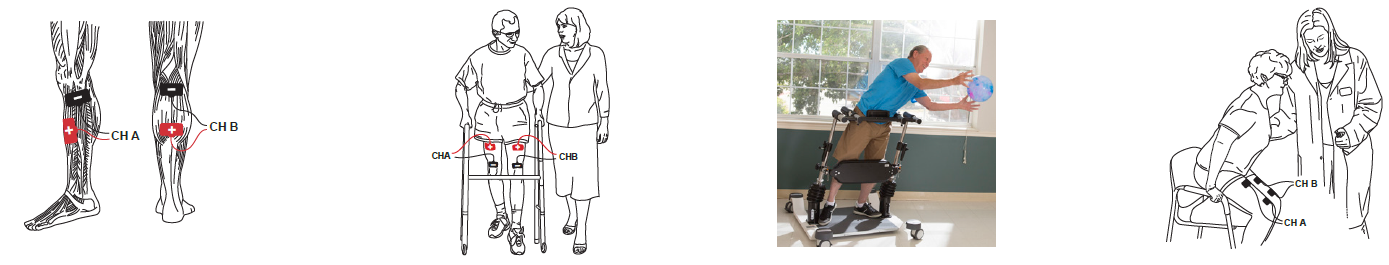
Heart disease is the leading cause of death for both men and women in the United States with greater than 600,000 deaths attributed each year. Along with other conditions such as diabetes and obesity, heart disease may lead to heart failure which affects 6.2 million Americans per year (CDC, 2020).
ACP
Recent Posts
Biophysical Agents and Advanced Technologies in the Rehabilitation of Patients with Heart Failure
Topics: Clinical Tip, Cardiopulmonary
Patient Information: Male, Age 91
Diagnosis: Parkinson’s Disease / Oropharyngeal Dysphagia /
COVID-19
History: This gentleman, a long-term resident of a skilled nursing facility, was diagnosed one and a half years ago with oropharyngeal dysphagia (difficulty swallowing), a complication of his Parkinson’s disease. Since that time he has had known aspiration (liquids entering the airway), altered diet, hospitalization for aspiration pneumonia, and COVID-19. Due to his complaint of his liquids being too thick, he requested to participate in swallowing therapy for possible return to thin liquids. As a result, swallowing evaluation and resultant therapy was initiated.
Topics: Dysphagia, Patient Success Story
Improving Strength and Functional Mobility with Electrical Stimulation and Exercise
Patient Information: Male, Age 75
Topics: Patient Success Story, Neuro Rehab
Patient Information: Male, Age 81
Diagnosis: COVID-19 / Acute Hypoxemic Respiratory Failure
History: This gentleman was referred to a skilled nursing facility for rehabilitation services due to severe debility and confusion after hospitalization for COVID-19. During hospitalization, he was found to have acute hypoxemic respiratory failure (not enough oxygen in the blood), as a result of COVID-19, and was intubated (placement of an artificial airway into the trachea) and placed on a ventilator (life support to assist breathing). During treatment he received convalescent plasma which led to removal of mechanical ventilation, but he required oxygen supplementation of three liters. Prior to his diagnosis of COVID-19, he lived at home with his wife and walked independently, no oxygen supplementation was needed.
Topics: Patient Success Story
Objective Tests and Measures: Strength Assessment and Treatment Guidance
Muscle strength decline is associated with normal aging and may be accelerated by illness, disease, or injury. Decreased physical activity resulting from COVID-19 mitigation efforts is exacerbating the incidence of muscle disuse atrophy in older adults. Strength declines may lead to functional and mobility deficits with increased risk of falls, injury, or death. According to the CDC, each year three million adults are treated in emergency departments for injuries related to falls. By 2030 fall deaths are anticipated to rise to seven per hour. Accurate assessment of strength using validated tests and objective measures is crucial to creating an appropriate treatment plan and achieving outcomes that reduce fall risk.
Topics: Fall Prevention & Balance, Clinical Tip, Cardiopulmonary
Topics: Industry News
Patient Information: Female, Age 72
Diagnosis: Cardiac Arrest / Pulmonary Embolism
History: This woman was referred to a skilled nursing facility for rehabilitation services due to severe weakness and debility following hospitalization. She had a pulmonary embolism (blood clot in the lungs) which required intubation and life support with extracorporeal membrane oxygen – ECMO (blood pumped outside the body to a heart and lung machine to remove carbon dioxide and send oxygenated blood back to the body). Prior to hospitalization, she lived at home and was independent with all mobility and self-care.
Topics: Patient Success Story, Cardiopulmonary
The rehabilitation of patients with and recovering from COVID-19 is evolving and will be an integral part of therapy for the foreseeable future. The American Physical Therapy Association (APTA) developed a task force representing all academies and sections to identify core outcome measures to be used with all patients diagnosed with COVID-19 throughout care, across all settings. These outcome measures are to be used with patients having goals associated with five constructs; function, strength, endurance, cognition, and quality of life. (APTA, 2020)
Topics: Clinical Tip, Cardiopulmonary
Decreasing Pain and Improving Functional Independence Using Electrical Stimulation and Exercise
Patient Information: Female, Age 76
Diagnosis: Chronic Heart Failure / Generalized Muscle Weakness / Shoulder Pain
History: This woman was admitted to the hospital to address multiple medical issues. Following hospitalization, she was referred to a skilled nursing facility for rehabilitation to address her limitations in strength and mobility, with a goal to return home alone at her prior level of function, independent with all mobility.
Topics: Patient Success Story
Improving Strength and Functional Mobility Using Electrical Stimulation and Exercise
Patient Information: Female, Age 68
Diagnosis: Respiratory Failure
History: This woman was referred to a skilled nursing facility due to severe deconditioning following a two-month hospitalization for pneumonia, during which she experienced respiratory arrest and required ventilation by tracheostomy intubation (surgical procedure inserting a breathing tube through the trachea to restore breathing).
Topics: Patient Success Story, Cardiopulmonary