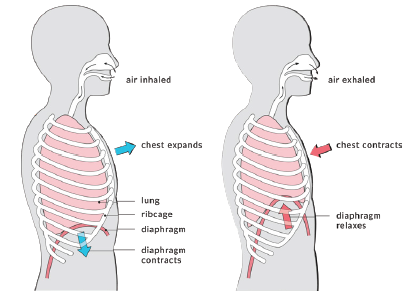
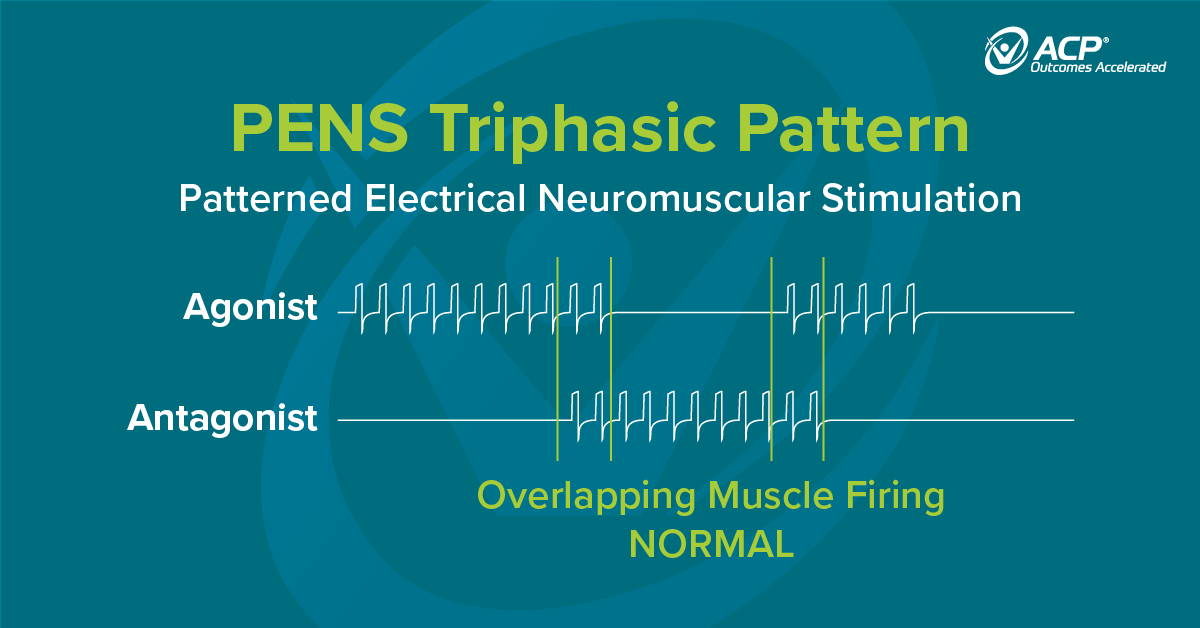
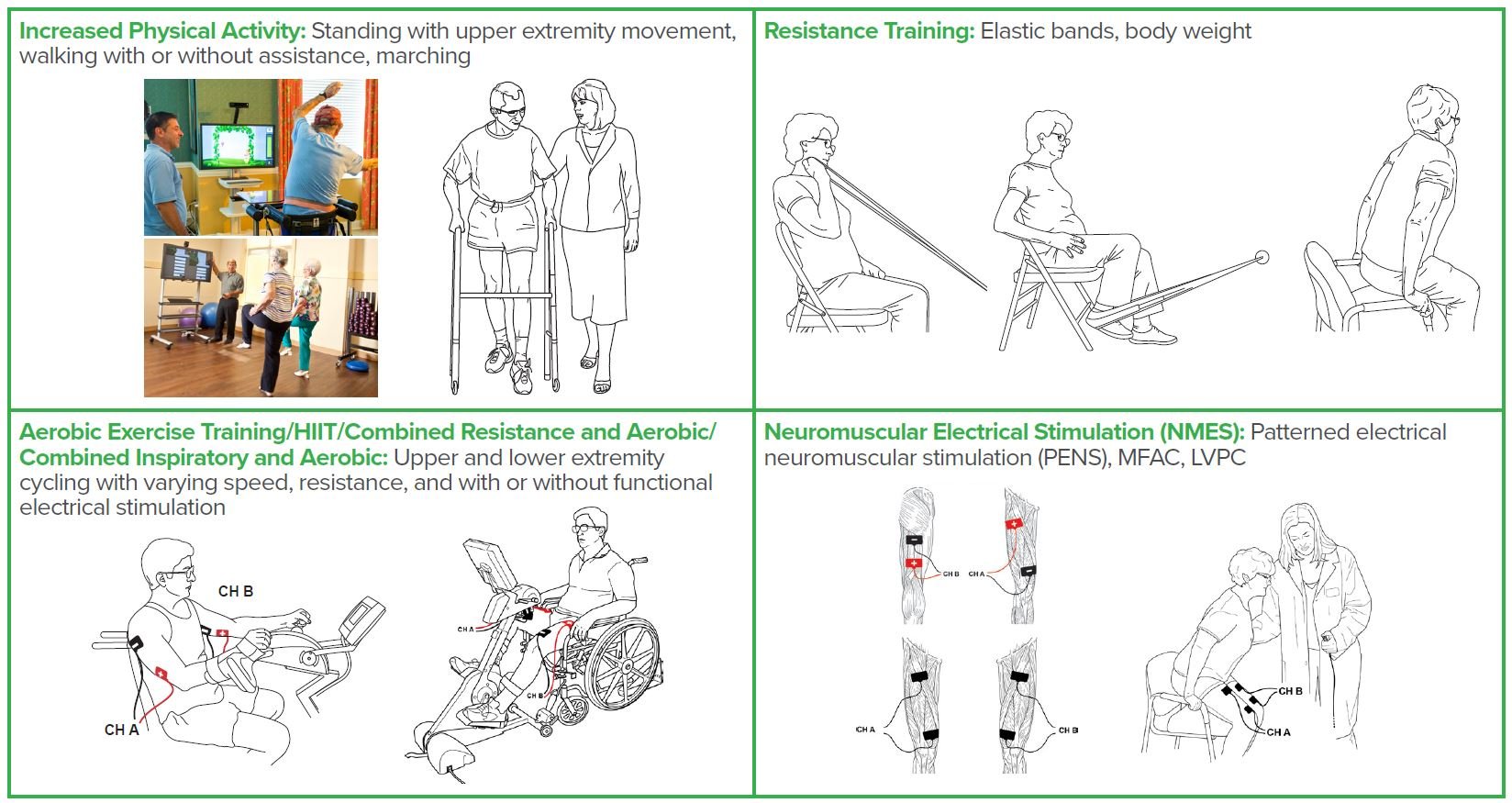
Diaphragmatic breathing helps individuals use their diaphragm correctly while breathing and enhances oxygen exchange (Cleveland Clinic, 2020). With age, stress, poor posture, and illness breathing changes and becomes shallow with increased reliance on accessory muscles. Implementing diaphragmatic breathing may help improve oxygen delivery throughout the body, use less effort and energy to breathe, and decrease overall oxygen demand.
ACP
Recent Posts
Diaphragmatic Breathing Exercise and Patterned Electrical Neuromuscular Stimulation (PENS)
Topics: Clinical Tip, Cardiopulmonary
Patient Information: Male, Age 65
Diagnosis: Stroke / Oropharyngeal Dysphagia
History: This gentleman was admitted to a skilled nursing facility for rehabilitation services following hospitalization due to a stroke. He was diagnosed with oropharyngeal dysphagia (difficulty swallowing). His swallow initiation was inconsistent and he had difficulty managing his own secretions. He could not take any food or liquid by mouth and a feeding tube was placed. Prior to his stroke, he ate a regular diet.
Topics: Dysphagia, Patient Success Story
Achieving Independent Functional Mobility with Electrical Stimulation, Diathermy and Exercise
Patient Information: Male, Age 69
Diagnosis: Chronic Heart Failure / Muscle Weakness / Kidney Failure
History: This man was admitted to a skilled nursing facility after a seven day hospital stay due to a decline in his ability to care for himself and his wife. He was referred to occupational and physical therapy to improve his strength and function, with the goal to return home and resume his role as the primary caregiver for his wife.
Topics: Patient Success Story, Cardiopulmonary
Improving Activation of Accessory Respiratory Muscles with NMES
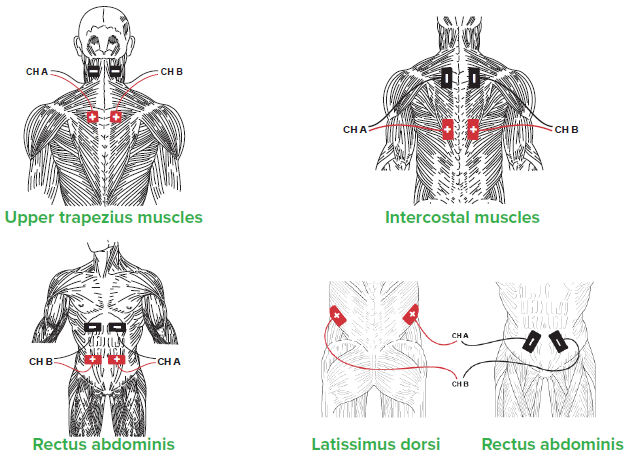
Primary respiratory muscles during normal quiet breathing include the diaphragm and external intercostals. Accessory muscles of respiration assist the primary muscles when the chest is not expanding or contracting effectively to meet ventilation demands. Increased age, stress, poor posture, COPD, pneumonia, and illness are conditions that negatively impact proper oxygen and carbon dioxide exchange in the lungs.
Topics: Clinical Tip, Cardiopulmonary
Rehabilitation for Severe Deconditioning Using Advanced Technology and Electrical Stimulation
Individuals who present with a compromised pulmonary system, are acutely ill, or hospitalized for extended periods may become deconditioned or develop hospital-acquired muscle weakness, among other deleterious effects. Even healthy individuals may become deconditioned and frail if they decrease their activity level due to social distancing and limiting time outside their room or home.
Topics: Clinical Tip, Cardiopulmonary
Improving Functional Mobility Using Electrical Stimulation, Virtual Reality, and Exercise
Patient Information: Male, Age 79
Diagnosis: Right Ankle Fracture / Gastrointestinal (GI) bleed
History: This gentleman was referred to a skilled nursing facility for rehabilitation services due to weakness and reduced functional mobility after hospitalization for a right ankle fracture (from a fall) and a GI bleed. Prior to hospitalization, he used a rolling walker to ambulate and lived in a 2-story home with a roommate who helped with household tasks.
Topics: Fall Prevention & Balance, Patient Success Story, Neuro Rehab
Infection control and patient safety are top priorities in healthcare. This document reviews low-level and intermediate-level infection control procedures for use with ACP technology to ensure the safety of healthcare providers and patients.
Topics: Clinical Tip
New evidence shows Patterned Electrical Neuromuscular Stimulation (PENS) effective in reducing knee pain and improving function
Two recent studies show that ACP’s proprietary PENS waveform technology is effective in treating patellofemoral pain (PFP) and improving muscle function during movement.
Topics: Pain Management, Orthopedic
Heart Failure Clinical Practice Guidelines Therapy Recommendations
Approximately 6.5 million adults in the United States have heart failure. Heart failure (previously referred to as chronic heart failure or CHF) occurs when the heart cannot pump enough blood throughout the body to meet the requirements of other organs and muscles. This results in a wide variety of symptoms and functional impairments which may result in hospitalization, re-hospitalization, and death. In 2017, heart failure contributed to 1 in 8 deaths. (CDC, 2020)
Topics: Clinical Tip, Cardiopulmonary
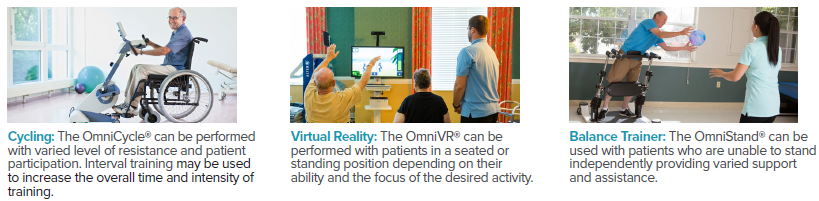
Over the past several years, the body of evidence on the effectiveness of virtual reality (VR) in rehabilitation has significantly expanded. VR has been studied for a variety of diagnoses including stroke, Parkinson’s disease, multiple sclerosis, dementia, burns, pain, and total knee arthroplasty. VR helps enhance patient involvement and motivation while increasing the repetitions and duration of exercise. Benefits addressing ADL performance, balance, gait, pain, and cognition have been reported.
Topics: Fall Prevention & Balance, Pain Management, Clinical Tip, Cardiopulmonary, Orthopedic, Neuro Rehab