Wounds are typically managed with standard nursing care including maintaining a clean wound bed and appropriate dressings and medications. Therapeutic interventions including biophysical agents can be used to directly facilitate and accelerate wound healing. Factors such as pressure, pain, and contracture may delay wound progression or cause wounds to reoccur. Addressing these adjunctive factors related to the wound provides the best overall approach to wound management and limits the risk of reoccurrence.
EPUAP/NPIAP/PPPIA, 2019 – Good Practice Statements:
• Reposition to offload bony prominences so that maximal redistribution of pressure is achieved.
• Use non-pharmacologic pain management strategies as a first line strategy and adjuvant therapy to reduce pain associated with pressure injuries.
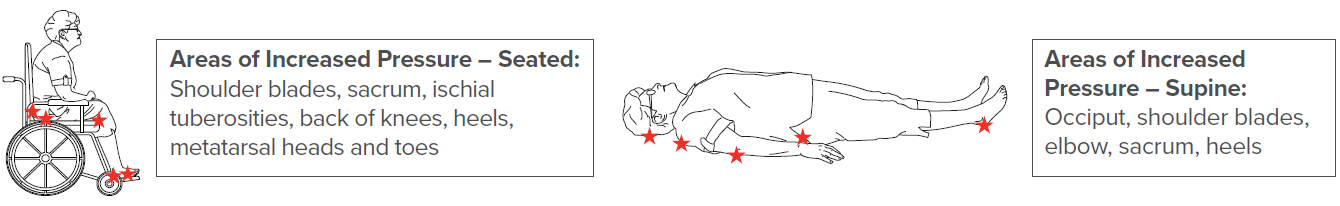
Pressure Relief:
Pressure injuries/ulcers (PI/PU) result when continual pressure on an area of the body occurs causing ischemia and tissue breakdown, typically over bony prominences. These areas should be inspected and pressure relief should be done regularly, passively (patient positioning, orthotics, surface changes) and/or actively (self-pressure relief techniques, movement).
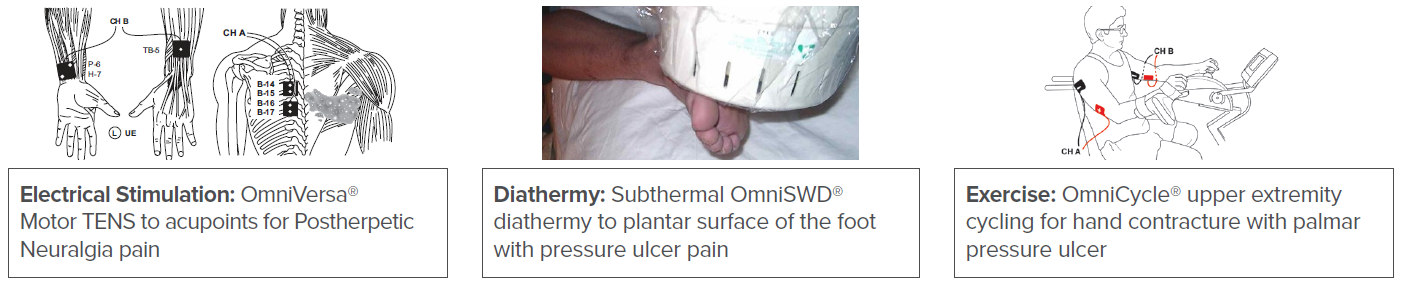
Pain:
Pain may be present due to the wound or prior to wound development due to factors such as pressure, injury, impaired circulation,
or a virus. Biophysical agents and exercise can be used to decrease pain and improve local tissue circulation.
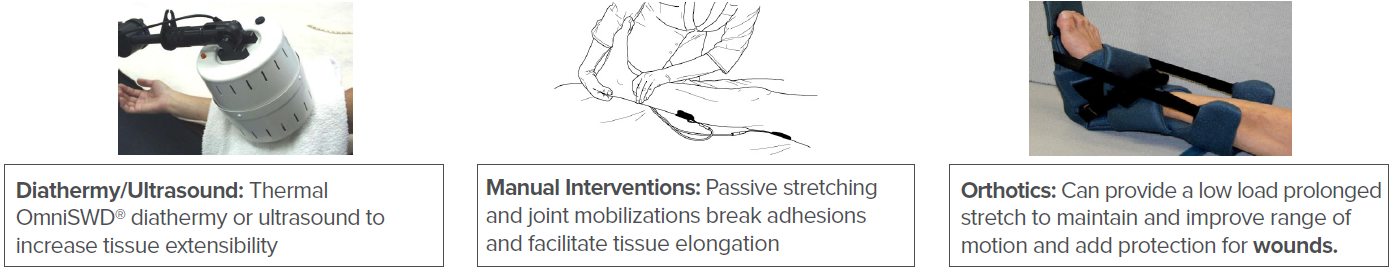
Contracture:
Contractures may develop prior to or after wound development. Biophysical agents, manual therapy, exercise, positioning, and orthotics can be used for contracture management. If hypertonicity is present, tone reduction strategies are necessary to make improvements. By addressing the contracture, improvements in range of motion, tissue healing, and reduction in risk of wound reoccurrence will be achieved.
Reference:
European Pressure Ulcer Advisory Panel (EPUAP), National Pressure Injury Advisory Panel (NPIAP), Pan Pacific Pressure Injury Alliance (PPPIA). (2019). Prevention and Treatment of Pressure Ulcers/Injuries: Clinical Practice Guidelines. The International Guideline. Emily Haesler (Ed.)
